Your cart is currently empty!
Navigating Insurance Coverage for Snoring Surgery
Navigating Insurance Coverage for Snoring Surgery: A Comprehensive Guide
Snoring is a common problem that affects millions of people worldwide. It not only disturbs the sleep quality of the snorer but also their partner and others who share the same space. While there are various remedies available for snoring, some people may require surgery to correct the underlying cause. However, the cost of snoring surgery can be expensive, and many individuals may wonder if their insurance will cover it. In this blog post, we will discuss everything you need to know about navigating insurance coverage for snoring surgery.
Understanding Snoring Surgery
Before discussing insurance coverage, it is essential to understand what snoring surgery is and what it entails. Snoring surgery is a procedure that aims to correct the underlying cause of snoring. It can involve various techniques, such as removing excess tissue from the throat, correcting structural abnormalities in the nose or throat, or using a continuous positive airway pressure (CPAP) device. The type of surgery recommended will depend on the individual’s specific condition and severity of snoring.
Insurance Coverage for Snoring Surgery
The first step in navigating insurance coverage for snoring surgery is to understand what your insurance plan covers. Most insurance plans cover medically necessary procedures, and snoring surgery may fall under this category if it is deemed essential for the individual’s health. However, some insurance plans may not cover snoring surgery, considering it a cosmetic procedure. Therefore, it is crucial to check with your insurance provider to understand what procedures they cover and the necessary steps to take to get coverage for snoring surgery.
Medical Necessity of Snoring Surgery
As previously mentioned, insurance companies will only cover medically necessary procedures. So, what qualifies snoring surgery as medically necessary? Snoring surgery is considered medically necessary if the individual has been diagnosed with a sleep disorder, such as obstructive sleep apnea (OSA). OSA is a severe condition that causes individuals to stop breathing temporarily while sleeping, leading to various health issues. If snoring surgery is recommended to treat OSA, it is more likely to be covered by insurance.
Documentation and Pre-approval
Before undergoing snoring surgery, it is crucial to gather all the necessary documentation to support the medical necessity of the procedure. This may include a referral from your primary care physician, sleep study results, and any other relevant medical records. It is also essential to check with your insurance provider if pre-approval or pre-authorization is required for snoring surgery. Some insurance companies may require pre-approval to ensure that the procedure is medically necessary before covering it.
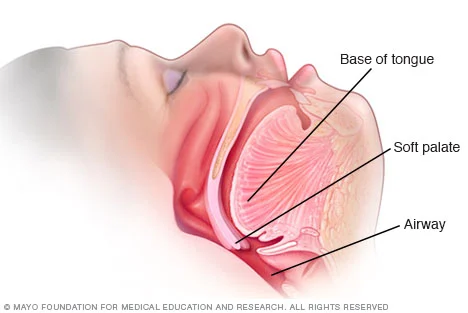
Navigating Insurance Coverage for Snoring Surgery
Out-of-Pocket Costs
Even if your insurance plan covers snoring surgery, there may still be out-of-pocket costs involved. For instance, your insurance plan may cover the surgery but not cover the cost of post-surgery care or medication. It is important to understand these costs beforehand and budget accordingly. Additionally, some insurance plans may require you to pay a certain percentage of the total cost of the surgery, known as a co-payment or co-insurance. Understanding these costs can help you plan better and avoid any unexpected expenses.
Alternative Treatment Options
In some cases, insurance companies may require individuals to try alternative treatment options before approving snoring surgery. These alternative treatments may include lifestyle changes, using a CPAP machine, or oral appliances. It is important to follow the insurance company’s guidelines and document the results of any alternative treatments. If these treatments are unsuccessful, it can strengthen the case for the necessity of snoring surgery.
Appealing a Denial of Coverage
In some instances, insurance companies may deny coverage for snoring surgery, considering it a cosmetic procedure or not medically necessary. If this happens, it is crucial to appeal the decision. The first step is to understand why the coverage was denied and gather any additional documentation that may support the medical necessity of the surgery. If the appeal is still denied, it may be necessary to seek help from a healthcare advocate or legal counsel.
In Conclusion
Navigating insurance coverage for snoring surgery can be a daunting process. However, with the right understanding and preparation, it can be made more manageable. It is essential to understand your insurance plan, gather all necessary documentation, and follow the guidelines set by your insurance provider. If coverage is denied, it is crucial to appeal the decision and seek help if necessary. Snoring surgery can greatly improve an individual’s quality of life, and with the right approach, it can be made more accessible through insurance coverage.
Summary:
Snoring surgery is a procedure that aims to correct the underlying cause of snoring. While it can be an effective solution for snoring, the cost of the surgery can be expensive. This blog post discusses navigating insurance coverage for snoring surgery, including understanding the medical necessity, documentation and pre-approval, out-of-pocket costs, alternative treatment options, and appealing a denial of coverage. By understanding these factors and following the necessary steps, individuals can make snoring surgery more accessible and affordable through insurance coverage.